Bone Loss in Teeth: What It Is, What Causes It, and What You Can Do About It
Most people know that teeth can decay or break. Far fewer people realise that the bone supporting those teeth can be lost — silently, gradually, and without obvious pain — until the damage is already significant.
Bone loss in teeth is one of the most clinically serious consequences of untreated gum disease, tooth loss and certain systemic conditions. It affects not just the stability of your teeth but the shape of your face, your ability to eat and speak comfortably, and your options for replacing missing teeth further down the line. It is also, in many cases, preventable — which is precisely why understanding it matters.
At Smile Perfections in Oadby, Leicester, led by Dr Juttes Pallipatt GDC No. 104499 and Dr Pratima Pallipatt GDC No. 101258, we see the effects of dental bone loss regularly — and we help patients understand their situation clearly and make informed decisions about what to do about it. This guide covers everything: what bone loss in teeth actually is, why it happens, how it is detected, what the consequences are if it progresses, and what modern dentistry can do to treat it.
What Is Bone Loss in Teeth?
Your teeth do not sit rigidly in the jaw like posts in concrete. Each tooth is suspended in a socket within the alveolar bone — the section of the jawbone specifically dedicated to housing and supporting the teeth. This support system includes not just the bone itself, but the periodontal ligament (thousands of collagen fibres that connect the tooth root to the bone) and the gum tissue surrounding it. Together, these structures are called the periodontium.
Bone loss in teeth — also referred to as alveolar bone loss or periodontal bone loss — occurs when the alveolar bone supporting one or more teeth is progressively destroyed. Once this bone is lost, it does not regenerate spontaneously in the way that, say, a broken arm heals. The body has limited ability to rebuild lost alveolar bone without professional intervention, and in many cases the loss is permanent without specific surgical treatment.
The consequences of this are significant. As the bone level drops, the support for the tooth diminishes. Teeth become mobile, drift out of position, and eventually — if the bone loss is severe enough — can be lost altogether. The gum tissue follows the bone level downward, creating what patients often describe as their teeth “looking longer” over time: this is gum recession, and it is a direct result of the loss of the underlying bone support.
What Causes Bone Loss in Teeth?
There are several causes of bone loss in teeth, but they are not all equally common. Understanding which applies to your situation is the starting point for the right treatment.
Gum Disease (Periodontal Disease)
By a significant margin, gum disease is the most common cause of bone loss in teeth. In the UK, the majority of adults have some degree of gum disease, and it is the leading cause of tooth loss in adults over 35.
Gum disease exists on a spectrum:
Gingivitis is the earliest and most reversible stage. Plaque accumulates along the gum line, causing inflammation, redness and bleeding when brushing. At this stage, the underlying bone has not yet been affected. Gingivitis is entirely reversible with professional cleaning and improved home care — no permanent damage has been done.
Periodontitis is the advanced stage where the infection extends beneath the gum line and begins to destroy the bone and ligament supporting the teeth. Pockets form between the tooth and gum, bacteria colonise below the gum line where brushing cannot reach, and the immune response to this chronic infection drives progressive bone destruction. This is where permanent damage begins.
The mechanism behind bone loss in periodontitis is important to understand: it is not the bacteria themselves that directly destroy the bone, but the host’s immune response. The body releases enzymes and inflammatory mediators in response to the bacterial infection, and it is these that break down the collagen fibres of the periodontal ligament and stimulate osteoclast activity — the cells responsible for resorbing bone. This is why periodontitis can progress even in people who brush regularly: if the infection below the gum line is not addressed professionally, the inflammatory process continues regardless of surface-level hygiene.
The critical and often unsettling feature of periodontal bone loss is that it is largely painless. The vast majority of patients with significant bone destruction around their teeth have no pain at all. By the time symptoms such as tooth mobility or abscess formation appear, the bone loss is typically advanced. This is the core reason why regular dental hygienist appointments and dental check-ups that include gum assessments are not optional extras — they are the primary mechanism by which bone loss is caught before it becomes irreversible.
Tooth Loss
When a tooth is lost and not replaced, the bone that previously supported it begins to resorb. This happens because the alveolar bone exists specifically to support the teeth: without the mechanical stimulation provided by a tooth root transmitting bite forces into the bone, the bone has no physiological reason to maintain its density and volume, and it is progressively reabsorbed by the body.
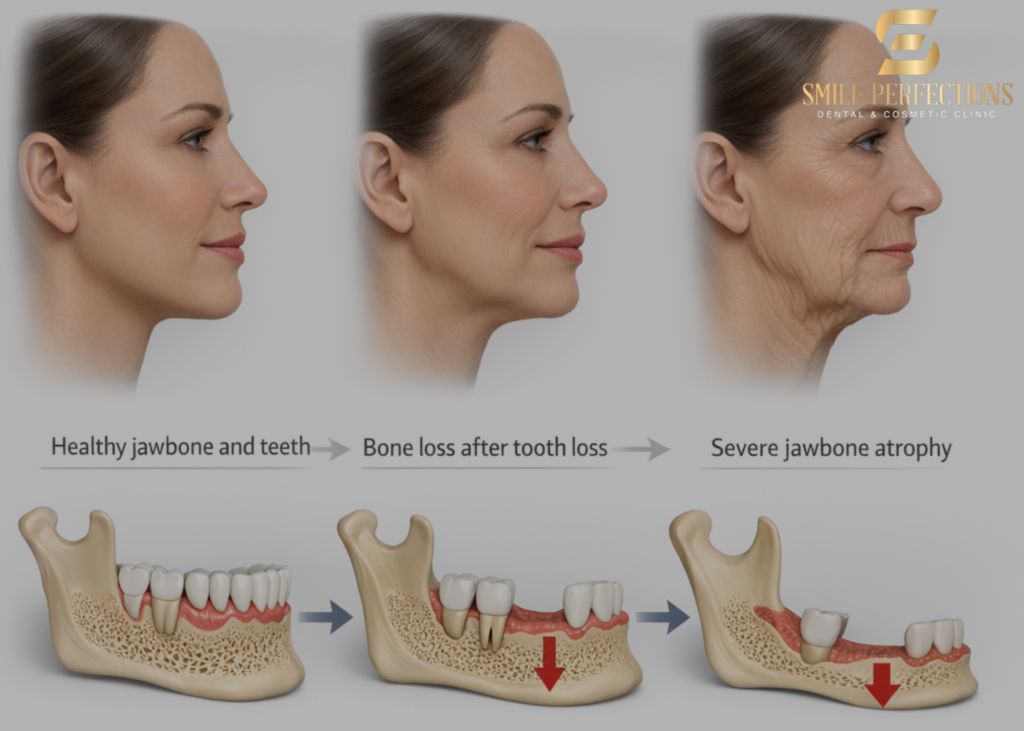
This process — known as disuse atrophy — begins within weeks of tooth loss and continues for years. In the first year after tooth loss, patients can lose up to 25 percent of the bone width at the extraction site, with bone height also diminishing over time. After ten years without a tooth replacement that engages the bone, the bone loss at that site can be dramatic.
This has two important implications: it changes the shape of the face (the lower third of the face can take on a collapsed, sunken appearance when multiple teeth have been lost and bone volume has reduced significantly), and it progressively limits the options for tooth replacement. Dental implants require adequate bone volume at the implant site, so the longer a tooth is left unreplaced, the more likely it becomes that bone grafting will be needed before implant placement — adding complexity, time and cost to the process.
Replacing missing teeth promptly — whether with a dental implant, a dental bridge or well-fitted dentures — is important not just for function and aesthetics, but specifically to manage and limit ongoing bone loss.
Ill-Fitting Dentures
Dentures sit on the gum surface and do not integrate with the bone beneath. Over time, as the bone continues to resorb (which happens under conventional dentures regardless, because the pressure they transmit to the ridge is not the same as the functional loading of a tooth root), the fit of the denture changes. An ill-fitting denture can apply uneven pressure to the gum ridge, accelerating bone resorption in localised areas and causing the denture to become progressively less stable.
This is a cycle: bone loss causes poor denture fit, and poor denture fit can worsen bone loss. Regular review of denture fit is important for this reason, and for patients with significant bone loss affecting denture stability, implant-supported solutions such as all-on-4 or all-on-6 implants can offer a transformative improvement.
Dental Infections and Abscesses
A dental abscess — a localised collection of pus caused by bacterial infection at the root tip or in the periodontal pocket — causes rapid and localised bone destruction if left untreated. The infection triggers an acute inflammatory response that can destroy significant amounts of supporting bone in a relatively short period.
Prompt treatment of dental infections is essential not just for pain relief but to limit the extent of bone damage. Once the acute infection is treated and resolved, the body can sometimes partially repair the resulting bone defect over time, though significant defects rarely resolve completely without surgical intervention.
Bruxism (Tooth Grinding)
Chronic tooth grinding places excessive and abnormal forces on the teeth and their supporting structures. While bruxism is not a direct cause of bone loss in the way gum disease is, the excessive occlusal forces it generates can accelerate bone loss in patients who already have reduced bone support due to periodontal disease. It also causes tooth wear, fracture and sensitivity, all of which compound the clinical picture.
Systemic Conditions
Certain medical conditions and medications are associated with increased susceptibility to bone loss in teeth:
- Osteoporosis: Reduced bone density throughout the skeleton is associated with a higher rate of alveolar bone loss and increased tooth loss risk, particularly in post-menopausal women.
- Diabetes: Both type 1 and type 2 diabetes are well-established risk factors for periodontal disease and accelerated bone loss. The relationship is bidirectional: poorly controlled diabetes worsens gum disease, and gum disease makes blood sugar harder to control.
- Smoking: Smokers have significantly higher rates of bone loss in teeth than non-smokers, partly because smoking impairs the immune response and blood supply to the gum tissue, and partly because it masks the classic warning signs of gum disease (such as bleeding) by constricting blood vessels in the gum.
- Long-term corticosteroid use: Can reduce bone density and increase susceptibility to periodontal breakdown.
HIV and immunosuppressive conditions: Impaired immune function increases susceptibility to aggressive forms of gum disease and associated bone loss.
How Is Bone Loss in Teeth Detected?
Bone loss in teeth is largely invisible to the patient and cannot be detected without clinical examination and radiographs. There are two primary diagnostic tools:
Periodontal Probing
During a full periodontal assessment, a calibrated probe is gently inserted into the gum pocket around each tooth and the depth is measured in millimetres at six points per tooth. Healthy gum pockets are typically 1 to 3mm deep. Pockets of 4mm or more indicate the presence of active periodontal disease, and depths of 6mm and above are associated with significant bone destruction.
This assessment — called a Basic Periodontal Examination (BPE) or full periodontal charting — is a standard part of a thorough dental check-up and should be carried out at every new patient examination and regularly in all adult patients. If it has never been done at your current practice, or if it has been a long time since a full gum assessment was included in your check-up, it is worth requesting one specifically.
Dental Radiographs
X-rays show the bone level around the tooth roots. In healthy periodontium, the bone sits close to the cemento-enamel junction (where the crown meets the root). Bone loss is visible on X-rays as a reduction in bone height — the bone level drops away from the tooth, exposing progressively more of the root surface.
Bitewing X-rays show the bone levels between teeth, while periapical X-rays show the full length of the root and the bone around the root tip. Panoramic X-rays (OPGs) give an overview of the whole dentition and jaw in a single image. Together, clinical probing and radiographic assessment give a complete picture of the extent and pattern of bone loss.
What Are the Consequences of Untreated Bone Loss?
The consequences of bone loss in teeth that is not treated promptly and appropriately range from uncomfortable to severely debilitating.
- Tooth mobility and tooth loss: As bone support diminishes, teeth begin to move under bite forces. Initially this may feel like slight looseness; as bone loss progresses, teeth shift out of alignment, bite problems develop, and eventually the remaining bone is insufficient to keep the tooth in function.
- Pain and abscess formation: While early bone loss is painless, advanced periodontitis and the abscess activity that can accompany it is often acutely painful and can cause facial swelling requiring urgent treatment.
- Facial changes: The alveolar bone contributes significantly to the shape of the lower face. Significant bone loss — particularly in the upper and lower front regions — causes the lips to lose their underlying support and the lower third of the face to appear sunken, aged and collapsed. This is most dramatically seen in patients who have worn full dentures for many years without bone support maintenance.
- Compromised options for tooth replacement: As bone volume decreases, the options for replacing teeth narrow. Patients with significant bone loss who want dental implants will often require bone grafting procedures before implant placement, which adds stages, time and cost to treatment. In some cases of very advanced bone loss, even grafting may not fully restore the original bone volume.
- Impact on overall health: The chronic inflammatory burden of untreated periodontal disease is associated in the research literature with increased risk of cardiovascular disease, adverse pregnancy outcomes, difficulties controlling blood sugar in diabetic patients, and other systemic conditions. The mouth does not exist in isolation from the rest of the body, and chronic infection and inflammation within it has consequences beyond the teeth themselves.
Treatment Options for Bone Loss in Teeth
Periodontal Treatment
The foundation of treating bone loss caused by gum disease is professional removal of the bacterial deposits driving the inflammatory process. This involves:
Scaling and root planing (root surface debridement): A deep cleaning procedure carried out under local anaesthetic in which the hygienist or dentist removes calculus (tartar) and bacterial biofilm from the root surfaces beneath the gum line. This removes the source of the infection, allows the gum tissue to reattach to the root surface and, in many cases, results in measurable bone gain in previously destroyed areas over the following months.
Dental hygienist appointments form the backbone of both the initial treatment and the long-term management of periodontal disease. Following an initial course of treatment, regular supportive periodontal therapy — typically every three to four months for periodontitis patients — is essential to prevent reactivation of the disease and further bone loss.
Surgical periodontal treatment: Where bone loss is advanced and scaling alone cannot adequately access the affected areas, periodontal surgery may be required. This can include flap surgery to improve access for cleaning, bone grafting procedures to regenerate lost bone volume, or guided tissue regeneration using membranes that encourage the body to regrow both bone and periodontal ligament in areas of destruction.
Replacing Missing Teeth to Preserve Bone
The single most effective way to prevent bone loss following tooth extraction is to replace the tooth with a dental implant. Because the titanium implant fixture integrates directly with the jawbone (a process called osseointegration) and transmits functional loading forces into the bone just as a natural tooth root does, the bone receives the mechanical stimulation it needs to maintain its density and volume.
Dental bridges are an effective tooth replacement option that restores chewing function and aesthetics, though they do not address the bone loss beneath the gap in the same way an implant does, since the pontic (false tooth) sits above the gum rather than integrating with the bone.
Dentures restore function and appearance but do not prevent underlying bone resorption. Implant-retained dentures, which use implant fixtures to anchor and stabilise the denture, provide better load distribution and can significantly slow ongoing bone loss compared to conventional removable dentures.
Full Arch Implant Solutions for Advanced Bone Loss
For patients who have experienced extensive tooth loss and significant bone loss across an entire arch, all-on-4 and all-on-6 implant solutions offer a pathway to a fixed, implant-supported set of teeth that can often be placed without the extensive bone grafting that individual implants might otherwise require.
The all-on-4 technique specifically is designed to work within the available bone by using strategically angled implants to engage the maximum amount of remaining bone. This has made fixed implant-supported teeth accessible to patients who were previously told they did not have enough bone for implants. At Smile Perfections, we assess each patient individually to determine which solution is most appropriate for their bone levels, overall health and functional needs.
Preventing Bone Loss in Teeth: What You Can Do
Prevention is always preferable to treatment, particularly for a condition where lost bone does not regenerate spontaneously. The most effective preventive steps are:
- Attend regular dental check-ups and hygiene appointments: A dental check-up that includes proper gum assessment is the only way to detect early bone loss before symptoms appear. Combining this with regular hygienist appointments to remove the subgingival bacterial deposits that drive the disease removes the primary cause at its source.
- Do not delay replacing lost teeth: The sooner a missing tooth is replaced — ideally with a dental implant — the less bone is lost at that site and the more straightforward the replacement process.
- Control systemic risk factors: Managing diabetes well, quitting smoking, and discussing with your GP any medications that may affect bone density are all relevant to managing bone loss risk.
- Maintain thorough home oral hygiene: While professional care is essential for sub-gingival disease, consistent brushing and interdental cleaning at home are the foundation that professional treatment builds on.
The Bottom Line
Bone loss in teeth is one of those conditions that does the most damage precisely because it causes so little discomfort in its early and middle stages. By the time patients notice that something is wrong — teeth moving, gaps appearing, dentures fitting poorly — the bone loss has often been progressing for years.
The good news is that caught early, treated properly and monitored consistently, even significant periodontal bone loss can be stabilised and the remaining bone preserved. And where bone loss has already led to tooth loss, the options available at Smile Perfections — from dental implants and bridges to dentures and full arch implant solutions — mean that there is a treatment path available whatever stage a patient presents at.
Dr Juttes Pallipatt and Dr Pratima Pallipatt and the team in Oadby take a thorough, honest approach to assessing and managing bone loss — starting with the kind of proper gum assessment and up-to-date X-rays that give a complete clinical picture, and working with each patient on a long-term plan that makes sense for them.
Patients frequently ask
It depends on the cause and the stage. Early periodontal bone loss that is treated promptly with professional cleaning and periodontal therapy can result in partial bone regrowth as the inflammation resolves and the tissue heals. More advanced bone loss typically cannot be fully reversed without surgical intervention such as bone grafting or guided tissue regeneration. Bone lost following tooth extraction will not regenerate on its own — a dental implant or bone graft is needed to restore volume. The most important message is that the earlier bone loss is caught and treated, the greater the potential for stabilisation and partial recovery.
Most patients with bone loss have no pain and no obvious symptoms until the condition is advanced. The only reliable way to detect it is through a proper periodontal assessment — gum pocket measurements at a dental check-up and dental X-rays that show the bone level around the roots. Warning signs that may prompt a check include bleeding gums, teeth that look longer than they used to, teeth that feel slightly loose, persistent bad breath, or gums that have receded visibly.
Yes — once a tooth is lost and not replaced, the bone that supported it begins to resorb. This starts within weeks of extraction and continues progressively. The rate of bone loss varies between individuals and sites, but it is an inevitable consequence of an empty socket. Replacing the tooth with a dental implant is the only replacement option that actively prevents this bone resorption, because the implant integrates with the bone and provides the same mechanical stimulation as a natural tooth root.
Conventional dentures sit on top of the gum and do not integrate with the bone beneath them, so they do not prevent ongoing bone resorption. Over time, as the bone continues to shrink, dentures become progressively less stable and well-fitting. Implant-supported dentures and all-on-4 or all-on-6 fixed implant solutions use implant fixtures that integrate with the bone, which significantly slows ongoing bone loss and provides the stability and confidence of a fixed or anchored prosthesis.
Patients with a history of periodontal bone loss typically require more frequent monitoring than patients with healthy gums. Three to four monthly dental hygienist appointments, combined with a thorough annual periodontal assessment that includes updated X-rays, is the standard recommendation for patients in periodontal maintenance. The frequency is determined by the stability of the disease: a patient who has been stable for several years may be able to extend intervals, while a patient with active disease will need more frequent care. Your dentist and hygienist will guide this based on your individual clinical picture.
Medical and dental information disclaimer
The information in this article is intended for general educational guidance only and does not constitute personalised dental or medical advice. If you are concerned about bone loss or your gum health, please book an appointment with a qualified dental professional for a full clinical assessment.
Smile Perfections is a private dental practice in Oadby, Leicester, led by Dr Juttes Pallipatt GDC No. 104499 and Dr Pratima Pallipatt GDC No. 101258. We offer a full range of dental treatments including dental check-ups, dental hygienist appointments, dental implants, all-on-4 and all-on-6 full arch implants, dental bridges, dentures, Invisalign, composite bonding, porcelain veneers, teeth whitening, dental crowns and smile makeovers.












